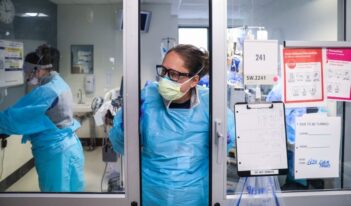
In the United States, immigration and administrative barriers hinder a valuable supply of health care workers.
The United States needs more health care workers.
The American Medical Association (AMA) estimates that the shortage of physicians could rise to as high as 139,000 by 2033. And a recent study shows that the shortage of nurses could rise to as high as 510,394 by 2030. Although no single factor explains this shortage, experts have pointed to the aging U.S. population and its growing health care needs, the high expense of medical training, increased levels of burnout, and issues related to funding for medical trainees.
International medical graduates (IMGs) are part of the answer to the U.S. health care worker shortage.
IMGs have supported the U.S. health care system for decades. They are physicians who received their medical degree abroad and came to the United States to finish their training or to join the U.S. health care workforce permanently.
The AMA reports that IMGs currently make up 25 percent of licensed physicians in the United States. This proportion has grown by nearly 18 percent over the past decade. A disproportionate number of IMGs work in internal medicine and geriatric medicine, two under-staffed specialties.
Despite their importance to the U.S. health care system, IMGs face a high administrative burden to qualify to practice medicine in the United States.
All IMGs must complete an accredited residency program in the United States or Canada, regardless of their training abroad. Physicians seeking to enter into a training program must get certified by the Educational Commission for Foreign Medical Graduates, a private nonprofit organization authorized to certify IMGs. The certification process takes an average of three years, during which time applicants must prove their medical school credentials and must pass two steps of the U.S. medical licensing examination.
IMGs who are not U.S. citizens or permanent residents also must obtain a visa. Many IMGs apply for a J-1 visa, a temporary visa available to applicants who participate in work or study exchange programs. The J-1 visa, though, only allows IMGs to remain in the United States for a maximum of seven years unless there is a documented need for an extension, after which time they are required to return to their home country for at least two years.
Under Section 214 of the Immigration and Nationality Act, this return requirement may be waived for up to 30 IMGs per state every year. This waiver, referred to as the Conrad 30 waiver program, is available to IMGs who are committed to working full-time for at least three years at a health care facility located in under-resourced, often rural, areas.
Some IMGs apply for an H-1B visa, which is a non-immigrant visa for specialized workers. To begin the H-1B visa process, the IMG’s employer must register with the Department of Homeland Security (DHS).
But H-1B visas are far from guaranteed. The application process is very competitive because the federal government receives far more applications than it is permitted to grant. When the number of applications surpasses the cap, DHS randomly selects petitions filed during the first five days of the registration period in a process called the “H-1B lottery.”
In 2020, DHS issued an interim final rule that put the H-1B lottery system at risk. Instead of randomly selecting applications, the interim final rule would allow DHS to rank and select the petitions with the highest wages.
Experts opposed the rule, arguing that it would have the highest impact on IMGs serving patients with the highest need, such as those in low-income and under-resourced communities. Last fall, a federal court struck down the rule, holding that DHS did not adhere to the requirements of the Administrative Procedure Act when it issued the interim final rule because it did not observe the appropriate notice and comment period.
Although the court set aside the DHS rule, under the lottery system, the agency continues to deny many H-1B applications.
In addition to residency and certification requirements, IMGs must also obtain a medical license from the state or states in which they intend to work. The state licensure requirements for IMGs are intended to mirror the requirements for domestic graduates, but the requirements are not uniform. All states, however, require at least one year of training at an accredited program in the United States or Canada.
Once IMGs are cleared to enter and work in the United States, they often face personal and institutional challenges. In a recent study, scholars explain that IMGs struggle to adapt to both residency and American culture. They also found that IMGs experience discrimination and are often undervalued by their peers. For example, one respondent in their study spoke about how some residents implied that IMGs were not as competent as American trainees.
Some experts argue that the problem with the U.S. health care system is not a lack of doctors, but a lack of administrative support and underuse of non-physician health care workers such as nurses, nurse practitioners, and physician assistants. Structural changes to the U.S. health care system may lessen the workload for health care professionals and improve patient care, but these changes will not relieve the emotional and administrative burden that IMGs currently face, nor will they obviate the need for IMGs in the United States.
IMGs are here to stay—and they can provide much-needed health care services in many parts of the United States. What, then, can be done to help them help us?
One way to help IMGs enter the United States is to amend the Conrad 30 waiver program. In 2019, U.S. Senator Amy Klobuchar (D-Minn.) introduced a bill to raise the cap on Conrad 30 waivers from 30 to 35 visas per state per year. And over the past two years, Congress has considered two other bills that recapture unused employment-based visas to increase the number of internationally trained physicians and nurses available to work during the pandemic. All of these bills have yet to move beyond committee.
Legislative action is part—but not all—of the support that IMGs need. To reduce the burden on IMGs, policymakers and health care administrators should work to accelerate the immigration process, simplify state licensure requirements, and change discriminatory policies and culture in the U.S. health care system.
After relying on their expertise for so long, America should acknowledge, value, and support IMGs.