Ireland’s Chief Nursing Officer endorses a flexible and compassionate approach to health care regulation.
Around the world, we are all dealing with the same issues, as the world is changing and regulation is becoming more complex. A key question we all face is: How do we prepare regulation for the future?
In Ireland, as we are on the cusp of major reform of our health system, we are in the process of implementing Sláintecare—our ambition to deliver a universal health service that offers the right care, in the right place, at the right time, at low or no cost. At the heart of Sláintecare is a shift to integrated primary and acute care, with multi-disciplinary teams of diverse professionals working together to deliver person-centered and coordinated care. Regulation will be a key enabler of our restructured health system.
We are finding we need to develop a more flexible approach to regulation that can respond and adapt to new ways of working. We are looking to the future of regulation and asking ourselves important questions around who we regulate, and why, and how “right touch” regulation can reinforce patient safety without imposing disproportionate barriers to health and social care professionals entering the workforce.
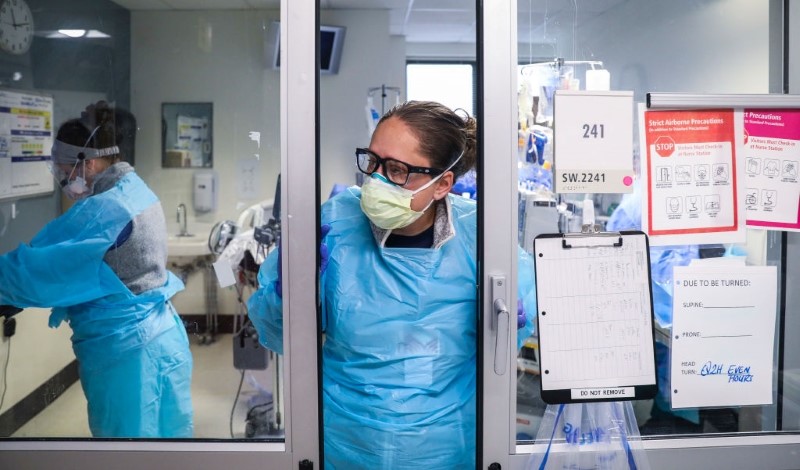
In Ireland, as I am sure may be the case elsewhere, our health care workforce is our biggest challenge. The COVID-19 pandemic changed Ireland, as it changed the world. It placed substantial strain on our health services, and our health care workers bore the brunt of that strain.
Many health care workers have reported feeling burnout. Staff well-being remains an ongoing concern. COVID also taught us that we are not immune to global trends and events. Like many countries, we are grappling with health care worker shortages, challenges in training the next generation of graduates, and difficulties in staff retention and recruitment.
Our health care workers, though, are our greatest asset in meeting the health needs of patients with kindness and compassion. Yet kindness can be in short supply with the stress and pressure health care professionals are under. I am therefore struck by the importance of emerging thinking about kindness and compassion in regulation itself.
Regulatory processes, such as fitness to practice, while so important, can also be a source of distress and deep dissatisfaction to health professionals and claimants alike. Wider societal attitudes about service and complaints have changed. As a result, we find ourselves challenged as regulators to ensure that our processes evolve to accommodate these changes. In particular, we need to shift our thinking to determine how we can support a more “just” culture which enables learning, focuses on improvement, and provides psychological safety for our workforce.
With the volume of fitness-to-practice complaints increasing, we need to find ways to embed compassion in our processes. This might involve greater scrutiny of the severity of complaints so as to differentiate the minor from the serious. We could strive to improve communication with professionals under investigation and complainants in ways that are more humane, respectful, and kind to all. We could strengthen collaboration across our health system and engage with employers, patient safety advocates, regulators, and others to address a blame culture that hinders learning and improvement. We could also look at pathways to embed learnings beyond the individual by thinking about the system more broadly.
Overall, we need to think differently and learn from each other about the ways in which we can incorporate kindness into our regulatory practice, to maintain our strong focus on patient safety while also protecting the well-being of our health care staff.
In Ireland, the Nursing and Midwifery Board is leading the way in this regard, having already incorporated the principle of kindness in its Code of Professional Conduct and Ethics for Nurses and Midwives. It is a start, but there is a lot more to do.
At the Department of Health in Ireland, we also have responsibility for professional regulation and patient safety. I can see the convergence of our thinking around patient safety. Concepts such as psychological safety can enable and support health and social care professionals to engage in effective teamwork and promote a more comprehensive approach to patient safety. We are working to create space for learning, encouraging self-awareness, and improving regular supervision and support.
We know that patients have a central role to play in the development of health policy and the reform of our health services, and that their voices must be listened to and heard. For this reason, the Department is currently in the process of developing a patient voice partner policy. This will ensure that patient participation is embedded in health policy decision-making and ensure that patients and service users participate in the design and delivery of Sláintecare reform.
Along with creating space for a stronger role for patients and their advocates in policy design and implementation, health and social care professionals have an important role to play in the policy space. In Ireland, we are fortunate to have health and social care professionals bringing their experience to regulatory policy. In addition to myself, the Chief Medical Officer, Chief Dental Officer, and a newly appointed Chief Health and Social Care Advisor have all practiced in our professions. We bring valuable understanding of how policy translates into practice.
The challenge that we as regulators must engage and confront is how to design regulation to be flexible enough to respond to health system needs and to keep people safe. Regulation can be seen as a “hard” tool. But we are increasingly building tools that will allow us to regulate in more agile and responsive ways.
Improved use of data has the potential to enable improved assessment and mitigate patient safety risk. Data can enable more robust evidence-based decision-making. Social media has already provided enough challenges for us in so many ways. And if that is not enough, innovation and advanced technologies will play an increasing role in the regulation space. We also need to have a discussion on what benefits and harms artificial intelligence may bring to professional regulation into the future.
We have challenges to address and plenty of opportunities to pursue. As regulators, we must reflect together on the major issues facing us as regulators and stakeholders in regulation. We need to collaborate, learn, engage, and be inspired.
This essay draws on opening remarks the author delivered at the Seventh International Congress on Professional & Occupational Regulation of the Council on Licensure, Enforcement, and Regulation in Dublin in May, 2023.




